News

What is an Iron Infusion? Benefits, Procedure, and What to Expect
Iron deficiency is a common condition where the body lacks enough iron to produce healthy red blood cells.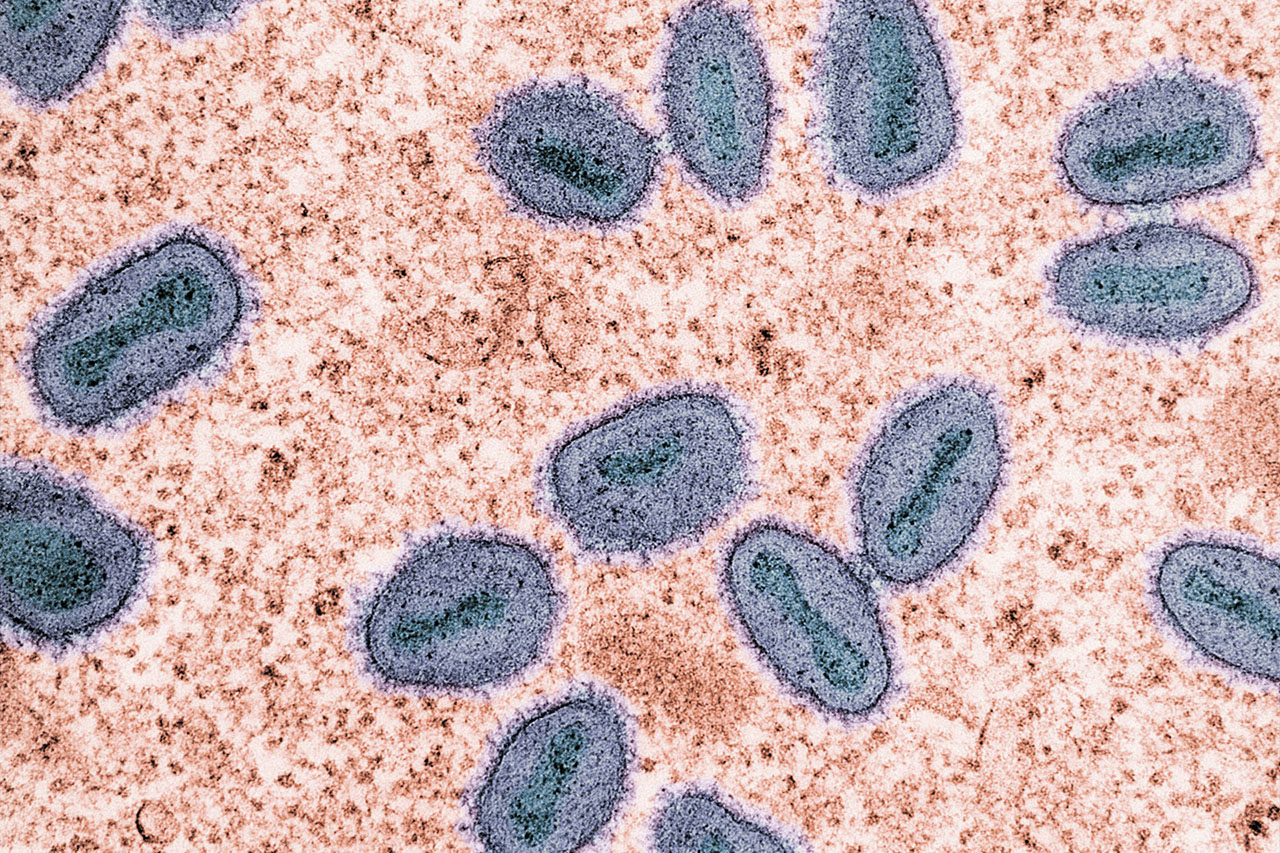
Mpox (Monkeypox) Information – Signs, Symptoms & Treatment
Mpox, formerly known as monkeypox, is a viral infection affecting Australia, primarily impacting GBMSM.
Heart Health And How You Can Improve It
Discover key steps to boost heart health and reduce heart disease risks. Learn about diet, exercise, and lifestyle choices for a stronger, healthier heart.
Top 7 Most Common Allergies
Discover the most common allergies in Australia, from food to latex. Learn their symptoms, triggers, and how to prevent them for a healthier life.
Sleep Myths | Let’s Put To Rest Some Common Myths About Sleep
We spend just under half of our life asleep so it's important you know the truth about sleep. Read our Sleep Myth busting guide here.
Thunderstorm Asthma
Thunderstorm asthma can happen suddenly to anyone, anywhere. Typically it occurs during the spring and summer.
Low Testosterone in Men
Discover the impact of low testosterone in men. Learn its causes, signs, and how it affects health. Get insights on treatments and ways to manage it.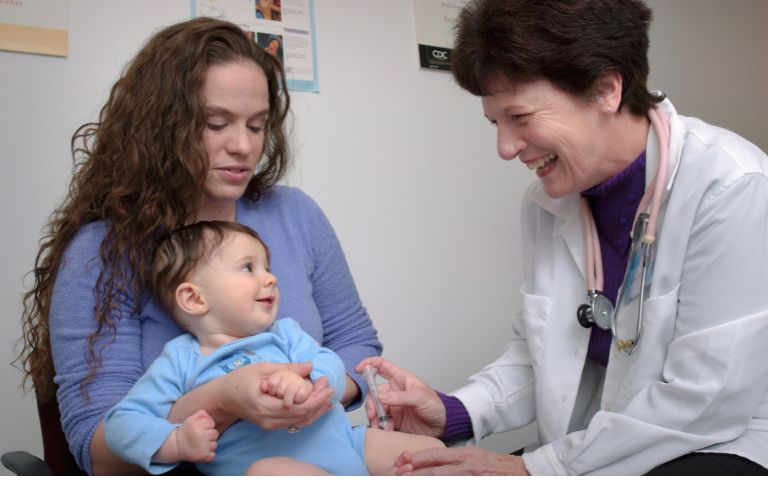
Preparing your Kid for Childhood Vaccinations
Prepare and comfort your child during vaccinations with essential tips, ensuring a smoother and less anxious experience for both of you.
What are the Causes For Blood in Semen?
Discover the reasons behind blood in semen, its implications, and potential treatments. Gain insights on related health concerns with Southgate Medical.
The Bad Effects Of Eating Junk Food
What you eat and drink each day effects your health and wellbeing, both physically and mentally. Find out about the negative side effects to eating junk food!
Medical Checkups – What should I be checking?
Learn why regular doctor visits, even when you feel fine, are important. Find out about different checkup types and how they keep you informed and healthy.