The future of the healthcare system is ever evolving as consumer demands shifts and the advancement of technology rises. More so there has been an increasing focus on personalized medicine in Australia in order to better predict risk for disease or patient responses to treatments. Personalized medicine takes into account genetics, genomics and any other biological information in order to make a well-informed decision regarding the diagnosis, prevention and treatment of human diseases in each patient. Data-driven analytics is revolutionizing the healthcare industry by applying what doctors have been doing for years but on a larger scale. The workings of new datasets and existing sciences of epidemiology and clinical medicine working hand in hand allow the healthcare industry to better understand relationships between external factors and human biology resulting in enhanced clinical treatments and truly personalized healthcare for the individual.
The medical benefits of personalized medicine are tremendous Australia wide, with significantly lower health costs through early prevention of diseases and more targeted treatments. The previous approach of prescribing medicine through a “one size fits all” or trial and error method is outdated as not everyone will react to a drug the same way. While the majority may respond well to a particular drug and dose, some patients may have very little effect or serious side effects from the same medication prescribed. In worst case scenarios it can lead to hospitalization and be a huge contributor to healthcare spending. Personalized healthcare views patients as individuals to help predict the right treatment and medicine with the fewest side effects. This can both tremendously improve the quality of care and decrease healthcare costs at the same time.
Personalized medicine, when coupled with behavioral economic principles, drives patient engagement. Many healthcare problems are behaviorally driven which means they can be potentially preventable. By getting patients involved in the care of their health we empower patients to take better care of their health. As we collect more data on individual’s risk for disease and response to treatment, we can convey this information to patients in order for them to better understand their treatment plan with more confidence based on facts and figures.
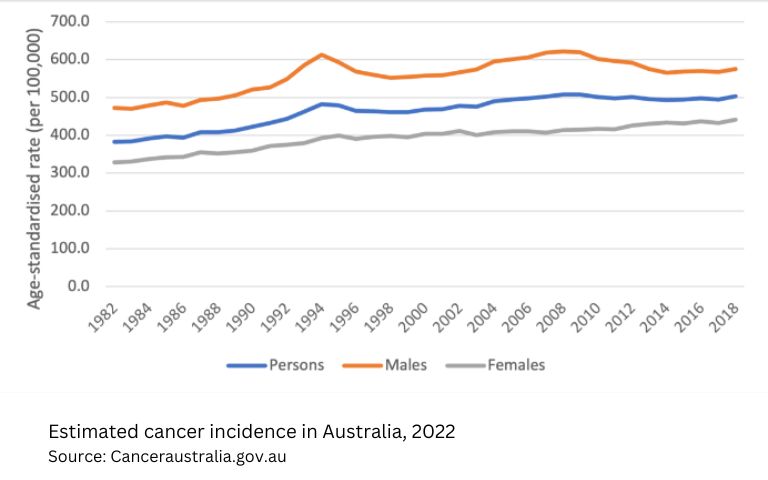
Development of Cancer Treatments
In the field of oncology, the impact of personalised medicine Australia wide is particularly evident; specifically targeted treatments are helping cancer patients live longer, healthier and more productive lives. Since the peak of cancer incidences in 1994, the cancer death rate (2014-2017) has increased by about 7.5% whilst the five-year survival rate (2009-2013) has climbed to about 68%.
Cancer is essentially a disease of altered genomics whereby there’s an influx of abnormal growth of cells. As each individual’s molecular makeup is different, every tumour is unique with genes made up of varying sequences of DNA. This explains why not every cancer patient will respond the same way to a treatment. Through genomic sequencing doctors can determine the DNA sequence that makes up the genome of each individual tumour in order to better diagnose what will be the most effective way to target the tumour. Personalised healthcare and personalised medicine is a customised treatment for each patient where targeted treatments are given and the patient’s responses are tracked over time. Cancer treatments that were once before heavily relied on traditional clinical trials are now moving to small sample or one-person trials in order to provide the most effective treatment.
As research develops on individual’s cancer cells, more cancer patients can potentially benefit from personalized approaches. Biomarkers (short for biological markers) play an important role in the prediction or diagnosis of various cancers and have been significant in the development of personalised healthcare. Biomarkers are biological molecules, cells or genes found in blood, other bodily fluids or tissue, that may be assessed to provide more information about a tumour (GI Cancer Institute). Epidermal growth factor receptor (EGFR) is a common biomarker for mutation in non-small cell lung cancer (NSCLC) patients. The presence of EGFR in a tumour suggests that these patients are more likely to respond to medicines that inhibit the EGFR pathway. Cancer biomarkers have enabled progress in the management of various tumours with notable biomarkers being HER2 for breast cancer, KRAS for colorectal cancer and ALK for lung cancer.
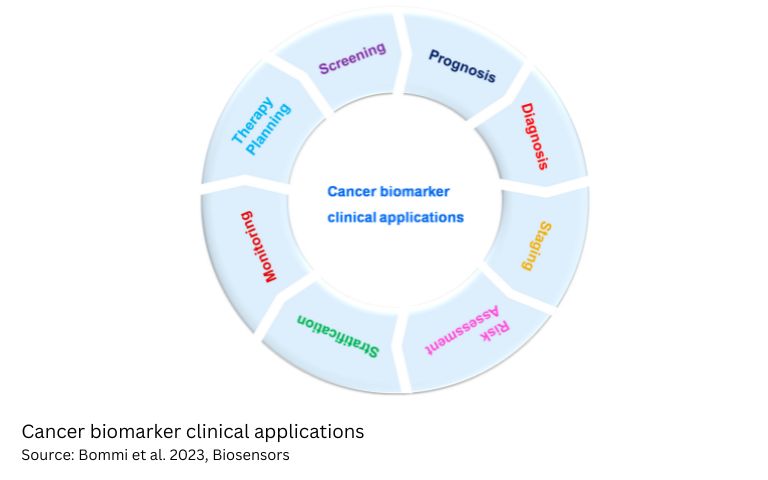
Personalised medicine is truly the future of healthcare with the potential to improve the overall survival rate for a range of cancer types and having a meaningful impact for patients.